Learn about Knee Therapy
Your knee has a cushion between the shinbone and thighbone known as a meniscus. The meniscus is prone to wear and tear and when it is torn it can be the source tremendous pain. At times the knee can lick and at times nothing happens but in case it does there will be need for therapeutic treatment.
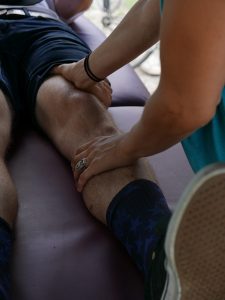 In a youngish person, when a knee-wrenching activity like skiing, ultimate Frisbee, or slipping on the ice tears a meniscus, the damage is often repaired surgically. But a torn meniscus is often seen in the 9 million Americans with knee osteoarthritis, and for them the best course of action hasn’t been crystal clear. Results of the Meniscal Tear in Osteoarthritis Research (MeTeOR) trial published yesterday in the New England Journal of Medicine indicate that physical therapy may be just as good as surgery.
In a youngish person, when a knee-wrenching activity like skiing, ultimate Frisbee, or slipping on the ice tears a meniscus, the damage is often repaired surgically. But a torn meniscus is often seen in the 9 million Americans with knee osteoarthritis, and for them the best course of action hasn’t been crystal clear. Results of the Meniscal Tear in Osteoarthritis Research (MeTeOR) trial published yesterday in the New England Journal of Medicine indicate that physical therapy may be just as good as surgery.
Meniscus tear2
When the shock-absorbing cartilage in the knee is torn by injury or worn ragged by use, the result is called a meniscal tear. Stiffness and a vague sensation that the knee is not moving properly often result.
Surgeons at Harvard-affiliated Brigham and Women’s Hospital and six other large hospitals recruited 351 men and women with symptom-causing knee osteoarthritis and a meniscal tear. Half completed a six-week physical therapy program aimed at easing inflammation, strengthening muscles supporting the knee, and improving the knee’s range of motion. The other half underwent a procedure called arthroscopic partial meniscectomy, in which unstable pieces of the meniscus are removed and the remaining edges are smoothed, followed by the same physical therapy program.
Participants in both groups reported similar improvements in knee function and pain at six and 12 months. About one-third of those who received only physical therapy “crossed over” during the course of the trial and had surgery.
Sourced from: http://www.health.harvard.edu/blog/physical-therapy-works-as-well-as-surgery-for-some-with-torn-knee-cartilage-201303206002
Even though you might be in pain there are situations where your pain is bearable. You can actually engage in some exercises that will help you heal your knee. One of these exercises is strengthening the butt and the other is stretching the muscles that support your knees.
- STRENGTHEN YOUR BUTTWe know from research that knee injuries, including common Anterior Cruciate Ligament (ACL) tears, can occur when large hip muscles are weak. ACL tears, which are eight times more likely in women athletes, have been shown to lead to other cartilage tears and are correlated with knee arthritis later in life.
As a society, our butt muscles are weak. When the main butt muscle (gluteus maximus) is weak, it causes the pelvis to drop and the upper thigh bone (femur) to fall inward. This imbalance creates painful downward stress on the hip, knee, and ankle every time you take a step.
Hip extensions are helpful exercises to strengthen the glutes. Learn why and how to properly do hip extensions in both standing and prone position in this clip from the Strong Knees DVD.
2. STRETCH THE MUSCLES THAT SUPPORT YOUR KNEES
When butt muscles atrophy or become imbalanced because we sit so much of the day, the hamstrings and hip adductors (inner thigh muscles) also overwork — to compensate for the underdeveloped gluteus maximus — resulting in compressive force on the knee joint. By stretching out these support muscles, you decrease the chance that they’ll get tight and cause muscle imbalances. So remember the complementary two-fold process: as you strengthen naturally weak muscles like the glutes, also stretch supporting muscles like the inner thigh muscles.
Sourced from:http://www.gaiam.com/discover/175/article/best-ways-ease-knee-pain-5-tips-physical-therapist/
At times knee injuries get serious and they cannot go away no matter the amount of therapy. In such a case the only last resort is surgery. This is the resort when medication is no longer effective in alleviating the pain. Your doctor of course has to examine and also allow the orthopedic surgeon to do the same to determine if you need surgery and when.
Knee replacement may be an option when nonsurgical interventions such as medication, physical therapy, and the use of a cane or other walking aid no longer help alleviate the pain. Other possible signs include aching in the joint, followed by periods of relative relief; pain after extensive use; loss of mobility; joint stiffness after periods of inactivity or rest; and/or pain that seems to increase in humid weather.
Your primary-care doctor may refer you to an orthopedic surgeon who will help you determine when/if it’s time for knee surgery and which type of knee surgery is most appropriate. Your surgeon may decide that knee replacement surgery is not appropriate if you have an infection, do not have enough bone, or the bone is not strong enough to support an artificial knee.
Signs that it might be time for a knee replacement:
Your pain persists or recurs over time
Your knee aches during and after exercise
You’re no longer as mobile as you’d like to be
Medication and using a cane aren’t delivering enough relief
Your knee stiffens up from sitting in a car or a movie theater
You feel pain in rainy weather
The pain prevents you from sleeping
You feel a decrease in knee motion or the degree to which you’re able to bend your knee
Your knees are stiff or swollen
You have difficulty walking or climbing stairs
You have difficulty getting in and out of chairs and bathtubs
You experience morning stiffness that typically lasts less than 30 minutes (as opposed to stiffness lasting longer than 45 minutes, a sign of an inflammatory condition called rheumatoid arthritis)
You feel a “grating” of your joint
You’ve had a previous injury to the anterior cruciate ligament (ACL) of your knee
Sourced from: http://www.zimmer.com/patients-caregivers/article/knee/who-needs-knee-surgery.html





